Umbilical Paraumbilical Hernias
Umbilical and paraumbilical hernias are types of hernias that occur in the area around the belly button (umbilicus).
These hernias develop when tissue, such as part of the intestine, protrudes through a weak spot in the abdominal wall near the umbilical region.
Umbilical hernias occur directly at the belly button, while paraumbilical hernias develop adjacent to the belly button. These hernias may cause discomfort, pain, and complications if left untreated.
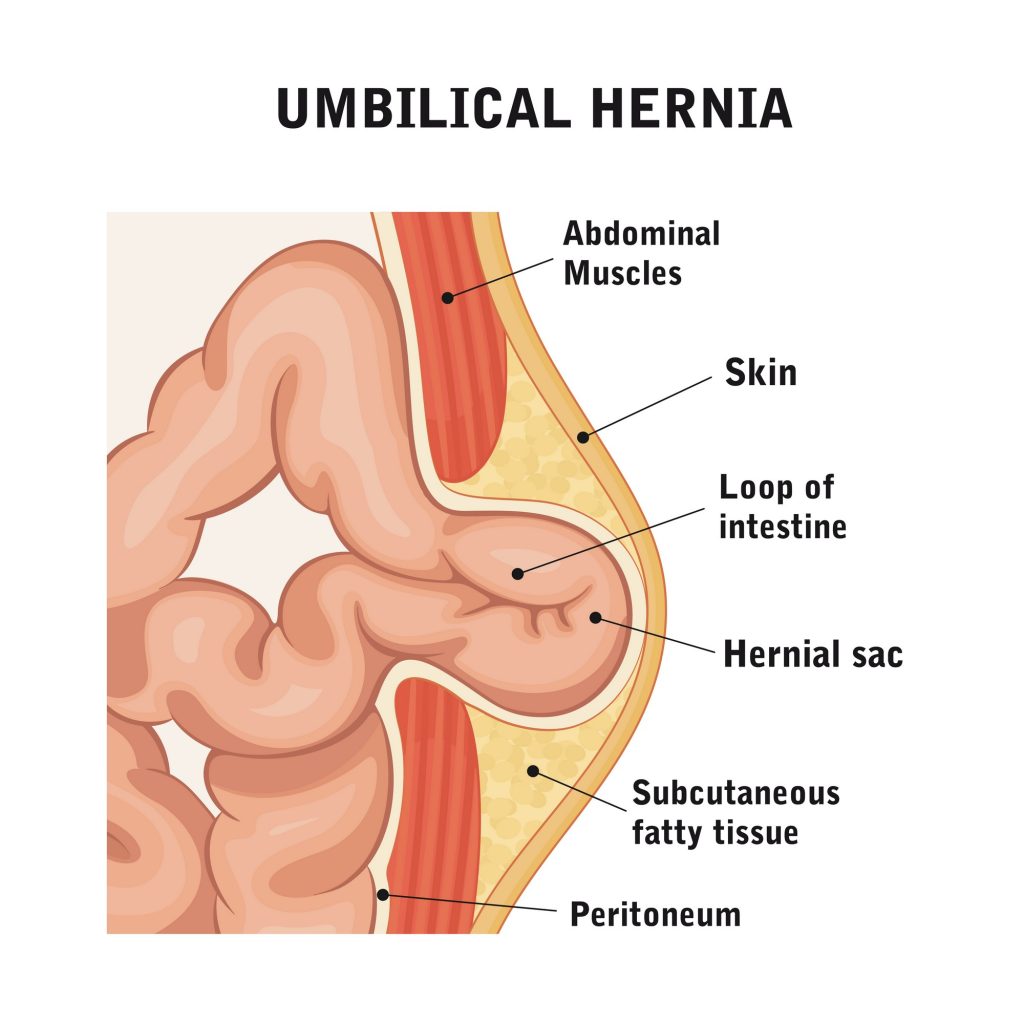
Causes and Risk Factors of Umbilical and paraumbilical hernias
The primary cause of umbilical and paraumbilical hernias is a weakening or stretching of the abdominal muscles and connective tissues in the umbilical region. Several factors may contribute to this weakening, including:
- Congenital Weakness: Some individuals may have a congenital weakness or defect in the abdominal wall that predisposes them to develop umbilical or paraumbilical hernias from birth.
- Pregnancy: Pregnancy can increase pressure within the abdomen and weaken the abdominal muscles, making women more susceptible to developing umbilical or paraumbilical hernias.
- Obesity: Excess body weight can put increased strain on the abdominal muscles and contribute to the development of hernias.
- Heavy Lifting: Activities that involve heavy lifting or straining, such as weightlifting or manual labour, can weaken the abdominal wall and increase the risk of hernia formation.
- Chronic Cough: Persistent coughing, such as that associated with smoking or lung conditions, can strain the abdominal muscles and contribute to the development of hernias.
Symptoms of Umbilical and paraumbilical hernias
The symptoms of umbilical and paraumbilical hernias can vary depending on the size and location of the hernia and whether any complications are present. Common symptoms may include:
- Visible Lump or Bulge: The most prominent symptom of umbilical and paraumbilical hernias is a visible bulge or lump in the umbilical region, which may become more noticeable when standing, coughing, or straining.
- Discomfort or Pain: Discomfort or aching sensation in the umbilical region, especially when lifting heavy objects, coughing, or bending over.
- Nausea and Vomiting: In some cases, umbilical and paraumbilical hernias may cause symptoms such as nausea, vomiting, or indigestion, particularly if the hernia compresses nearby organs or disrupts digestive function.
- Tenderness and skin change: The area around the hernia may be tender to the touch and red, especially if the hernia becomes inflamed or incarcerated (trapped).
- Change in Bowel Habit: In rare cases, large umbilical and paraumbilical hernias may compress the intestines or disrupt bowel function.
Diagnosis of Umbilical and paraumbilical hernias
Diagnosing umbilical and paraumbilical hernias typically involves a physical examination and may include additional imaging tests. Common diagnostic methods may include:
- Physical Examination: A healthcare provider may perform a physical examination to feel for a lump or bulge in the umbilical region and assess its size, location, and reducibility (whether it can be pushed back into the abdomen).
- Ultrasound: An ultrasound scan may be used to visualize the hernia and surrounding structures to confirm the diagnosis and assess for any complications.
Treatment of Umbilical and paraumbilical hernias
Treatment for umbilical and paraumbilical hernias depends on the size, location, and severity of the hernia, as well as the presence of symptoms or complications. Treatment options may include:
- Watchful Waiting: In cases where the hernia is small, asymptomatic, and not causing complications, a healthcare provider may recommend watchful waiting and monitoring for any changes in size or symptoms.
- Laparoscopic Surgery: In some cases, minimally invasive laparoscopic surgery may be performed, involving small incisions and the use of a camera and specialized instruments to repair the hernia.
- Robotic Surgery: Minimally invasive surgery using small (8mm) incisions and attached to robotic instruments (controlled by the surgeon) can be appropriate in some patients with umbilical/ paraumbilical hernia. Most patients are served well by either the laparoscopic or open approach.
- Open Surgery: Traditional open surgery may be necessary for larger or more complex hernias, involving an incision in the abdomen to access and repair the hernia with either stitches or mesh.